What is Subungual Melanoma?
Nails are adjoining structures of the skin located in the distal regions of the limbs, consisting primarily of hardened dead cells that contain a fibrous protein called keratin. Nails can be affected by pathologies of the skin and the integumentary system, but they can also be affected as part of systemic diseases.
We must differentiate the following categories:
- Ungual melanoma: melanoma that originates from below the surface of the nail.
- Subungual melanoma: melanoma from the matrix of the nail.
- Periungual melanoma: melanoma that originates from the skin next to the nail plate.
How Common is Subungual Melanoma?
Subungual melanoma is a very infrequent cancer, accounting for approximately 5% of all cases of melanoma. Usually, it is located on the thumb and the big toe. The average age of people affected by this type of cancer is between 60 and 70 years old. Then, subungual melanoma is a rare pathology that, due to a late diagnosis, it is complex to predict. Sometimes it is confused with a subungual hematoma, which is a common trivial pathology. Therefore, subungual melanoma is the most common type of melanoma diagnosed in highly pigmented individuals.
Symptoms of Subungual Melanoma
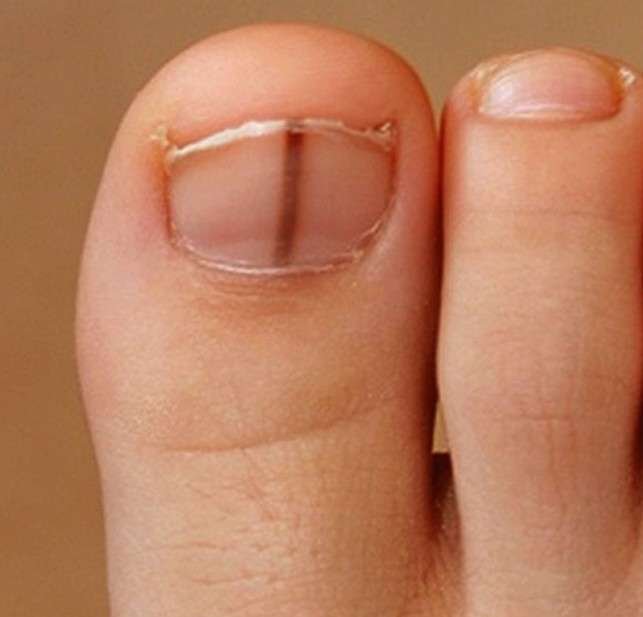
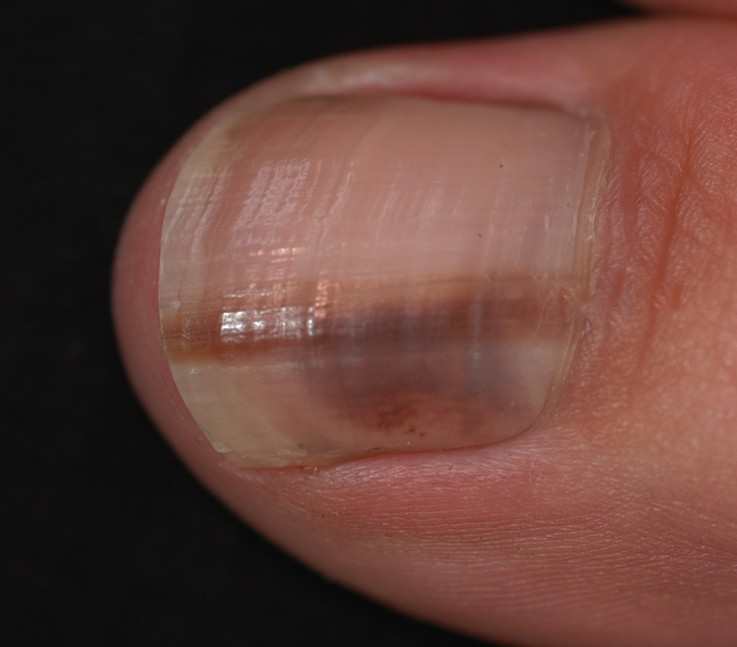
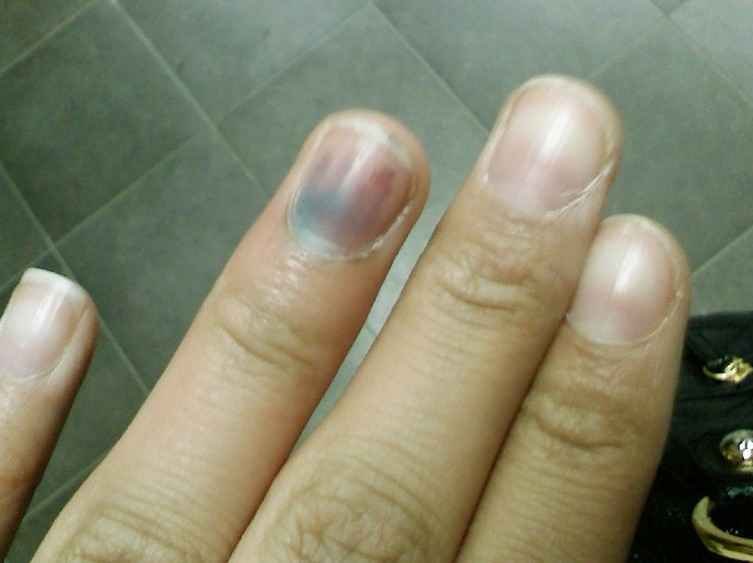
The symptoms of subungual melanoma are often difficult to diagnose, because their incidence is in a relatively unknown place. Subungual melanomas often appear as a dark line below the nail. However, since the predisposition of the condition happens in people with dark color skin, such lines underneath the nails are usually normal and benign. In the event that the stripe changes shape or color, or if a new stripe appears, it is advisable to consult the medical professional. Other indications of advanced subungual melanoma are damaged nail beds, or skin hyperpigmentation. The first signs and symptoms of subungual melanoma are often the development of a new pigmented growth or unusual appearance on the skin or nails.
Melanomas can grow in areas of the body with little or no exposure to the sun. They are named occult melanomas. When melanoma arises in people with darker skin, it is more likely to happen in a hidden area of the body. Subungual melanoma begins under the nail, and it can affect hands or feet. The first sign of a subungual melanoma is usually a brown or black coloration, often confused with a contusion.
What Causes Subungual Melanoma?
Subungual melanoma is more common in Native American, African American, and Asian individuals. It usually has a brown-black pigment, and a blurred border. When melanoma changes, it means size increase and / or growth speed of the nail or the pigment. When there is no apparent change, we speak of nail dystrophy, which person does not improve despite an adequate treatment. Subungual melanoma extension affects to the pigmentation to the proximal or lateral nail fold (Hutchinson’s sign), or to the free edge of the nail. The family clinical history of melanoma (or personal clinical history), as well as dysplastic nevus syndrome, are determining factors in the appearance of the subungual melanoma, since the probability of developing this cancer increases significantly. Professional medical research does not consider the development of this cancer due to prolonged exposure to the sun.
Medical and health professionals have found evidence linking subungual melanoma and trauma. 58% of subungual melanoma of the hand is located in the thumb, and 86% of the subungual melanoma of the foot is located in the first finger, probably because of the larger size of the nail bed (more melanocytes), also because they are the more exposed to trauma fingers. The morphology can be very variable, from a longitudinal brown band (longitudinal melanonychia), to a destruction of the nail articulation, or macular lesions in the nail bed extending from the matrix. Up to 20% of subungual melanoma are amelanotic, making diagnosis especially difficult.
How fast does Subungual Melanoma grow?
Subungual melanoma often begins as a visible pigment band on the length of the nail plate (melanonychia). For weeks or months, the pigment band:
- Grows, especially in the proximal termination (cuticle).
- Becomes more irregular in pigmentation, including light brown and dark brown.
- Extends by becoming involved in the adjacent nail fold (Hutchinson’s sign).
- Can develop a lump, ulcerate or bleed.
- Can lead to thinning, cracks or deformation of the nail plate (nail dystrophy).
However, up to half of all cases of subungual melanoma are amelanotic (non-pigmented). Nail melanoma may form a lump under the surface of the nail, lifting it (onycholysis). Sometimes it may look like a verrucous wart. It is usually painless, but the advanced tumor invades the underlying bone, which can origin a grim pain.
Diagnosis
The differential possible diagnosis includes: paronychia, keratoacanthoma, pyogenic granuloma, glomus tumor, nevus, fibroma, exostosis, onychotillomania, radiodermitis, onychomycosis and carcinomas. Before a doubtful hematoma, medicine doctors can observe it for 4-6 weeks to check if it moves with the growth of the nail, with no extension in the surface. If this is not the case, the biopsy should be done.
The prognosis of subungual melanoma is worse than cutaneous melanoma, due to its late diagnosis. Thus, early diagnosis is more important because it enables curative treatment. The primary care physician must know deeply the characteristics of subungual melanoma to be able to identify this disease.
Subungual melanoma can be diagnosed clinically because of a new or changing pigment stripe in a single nail. The dermoscopic examination may reveal more details showing pigmented lines of varying color, width and spacing. These lines tend to lose their usual tendency to run parallelly with each other along the length of the nail. When the clinical diagnosis is subungual hematoma (a purple mark underneath the nail due to bleeding or bruising), the nail may be observed for a few weeks. Nails of normal appearance should grow behind the mark. Dermoscopy is useful when the hematoma does not fit the pattern of subungual melanoma. However, it is important to remember that melanoma can bleed.
Treatment
Treatment for subungual melanoma is usually a surgery that depends on the stage and severity of the disease. If the melanoma does not have a depth greater than 1 mm, a local excision is all that is needed. However, if the depth is greater than 1 mm, excision in addition to a lymph node biopsy is recommended. In case if melanoma is overly advanced, surgical subtraction of the hand (or foot) finger may be required. In cases where surgery is not completely effective, chemotherapy may be used. Chemotherapy consists of drugs that fight cancer by attacking and destroying cancer cells.
The major factor associated with the risk of melanoma spreading (metastasis), and the probability of death, is the thickness of the melanoma at the time of complete elimination of the primary tumor. Delayed diagnosis is common in the case of subungual melanoma, especially when this cancer affects the tip, and some of these tumors have already spread at the time of diagnosis. The 5-year survival rate is very varied from 16% to 87%, depending on the stage of the melanoma. This is the most important reason for an early and accurate diagnosis.
In summary, the treatment of this cancer depends on several factors, such as the general health stage, and the stage at which melanoma was predicted. At an early stage, treatment usually involves surgery to remove melanoma. In case of melanoma has outspread out there the skin, other treatments consist of: Accurate Surgery to extirpate affected lymph nodes. Additional treatments before or after surgery may also be recommended.
Chemotherapy uses drugs to kill cancer cells. Chemotherapy can be given intravenously, by pills, or both, to encompass the entire body. Chemotherapy may be given into an arm or leg vein in a procedure named isolated member perfusion. During this procedure, arm or leg blood cannot reach other areas of the body for a short time, in order to the chemotherapy drugs reach the area around the melanoma without affecting rest of the body regions.
Radiation therapy is a treatment that uses high-energy energy rays, such as x-rays, to destroy cancer cells. It is sometimes used to help relieve the symptoms of melanoma that has spread to another organ.
Biological therapy stimulates the immune system to help fight the cancer. This medical treatment consists of elements produced by own body, or similar developed in a clinical laboratory. Biologic therapies used to treat melanoma include interferon and interleukin-2. Side effects of these treatments are similar to those of the flu, including chills, fatigue, fever, headache and muscle aches. Ipilimumab is another medicine that uses the immune system to fight melanoma. Ipilimumab is used to treat advanced melanoma that has spread beyond its original location.
Subungual Melanoma Pictures
Take a look at some of thepictures of Subungual Melanoma to see how the condition looks like: